
CRF has been applied for the treatment of cervicogenic headaches, occipital neuralgia, cervical radicular pain, lumbar radicular pain, discogenic pain, and pain associated with the sacroiliac joint. This review aims to show how PRF on dorsal root ganglion (DRG) is usually performed and its potential mechanisms of action and to summarize the most relevant currently available results in the literature.ĬRF to DRG is a heat destructive technique that has been used for more than 30 years for the treatment of chronic pain: CRF exposes target nerves to a continuous electrical stimulation that increases the temperature around the needle tip (between 60☌ and 80☌), thus destroying the fibers that conduct the nociceptive input. PRF has shown promising results in many fields of application, including different spinal pain condition like cervical radicular pain, posterior degenerative spinal disease, disc-related pathology, sacroiliac joint pain, spondylolisthesis, and infection. Thus, PRF is based on a different mechanism of action from conventional continuous radiofrequency (CRF), where temperature easily rises above this critical value because of continuous administration, inducing tissue heating and thermal coagulation. Pulsed radiofrequency (PRF) is a relatively new noninvasive technique that relies on the intermittent administration of high-frequency current, avoiding temperature to rise beyond the critical level of 42☌, described as the threshold for neuronal damage. 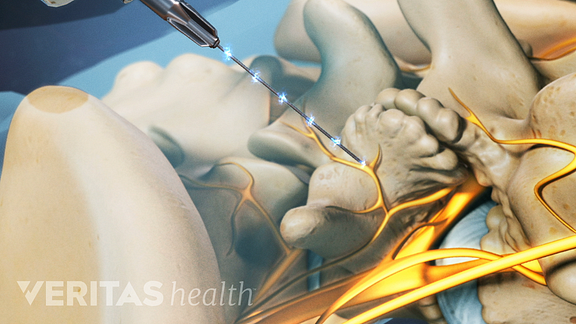
Moreover, surgery is associated with several side effects. Surgery provides for a better short-term pain relief as compared to prolonged conservative care, but no significant differences have been found between surgery and conservative treatment after one or 2 years. Surgery (discectomy, microdiscectomy, and other microsurgical techniques) is usually recommended in selected patients with severe symptoms and no benefit from conservative treatment, or in case of major neurologic impairment. Transforaminal injection (TFESI) under radiological guidance seems to be more effective than epidural injection. Įpidural corticosteroid injection has been widely used in clinical practice for many years, but it should be recommended as a means of reducing pain in the short term although no long-term effects can be expected, with a complication rate ranging between 0% and 9.65%. Noninvasive non – pharmacological interventions, which consist in physical exercise (biomechanical, aerobic, mind-body or a combination of approaches) with or without manual therapy (spinal manipulation, mobilization, and massage) or psychological therapy have outcomes that are often not long-lasting. Medication (paracetamol, NSAIDs, opioids) is a possible option for the treatment of radicular pain, but there is a lack of evidence to support the prescription of any particular drug. The presence of nerve root problems is an indicator of possible underlying pathology : the most common cause of lumbar radicular pain is intervertebral disc herniation (DH), followed by failed back surgery (FBSS) and spinal stenosis (SS). Ībout 90% of patients with low-back pain will have symptoms without a clear-specific cause. The annual prevalence of low-back pain with leg pain traveling below the knee lies between 9.9% and 25%. 
Low-back pain is usually defined as pain, muscle tension, or stiffness localized below the costal margin and above the inferior gluteal folds, with or without leg pain (sciatica).
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
